Recent Trends
- Home
- Recent Trends
Hearing, Ear Infections, and Deafness
Diseases and Conditions That Can Cause Deafness :
- uditory Neuropathy
- Auditory Processing Disorder
- Ear Infections—facts for parents
- Ear Infections (Otitis Media)
- Enlarged Vestibular Aqueducts (EVA)
- Hearing Loss/Deafness, Sudden
- Hearing Loss in Adults Over 60
- Hearing Loss, Noise Induced
- Hearing Loss, Ten Ways to Recognize
- Miniere’s Disease
- Otosclerosis
- Pendred Syndrome
- Presbycusis—age-related hearing loss
- Ringing in the Ear (Tinnitus)
- Usher Syndrome
- Vestibular Schwannoma and Neurofibromatosis
- Waardenburg Syndrome
For New Parents
Baby’s First Hearing Screening—within 1st month
Baby’s Hearing Screening Follow-up Checklist—birth to 6 months
Checklist for Your Child’s Hearing Development—birth to 3 years
TINNITUS ( RINGING IN THE EARS )
Do you hear a ringing, roaring, clicking, or hissing sound in your ears? Do you hear this sound often or all the time? Does the sound bother you a lot? If you answer yes to these questions, you may have tinnitus.
Tinnitus is a symptom associated with many forms of hearing loss. It can also be a symptom of other health problems. Roughly 25 million Americans have experienced tinnitus. Some cases are so severe that it interferes with a person’s daily activities. People with severe cases of tinnitus may find it difficult to hear, work, or even sleep.
- Hearing loss. Doctors and scientists have discovered that people with different kinds of hearing loss also have tinnitus.
- Loud noise. Too much exposure to loud noise can cause noise-induced hearing loss and tinnitus.
- Medicine. More than 200 medicines can cause tinnitus. If you have tinnitus and you take medicine, ask your doctor or pharmacist whether your medicine could be involved.
- Other health problems. Allergies, tumors, and problems in the heart and blood vessels, jaws, and neck can cause tinnitus.
The most important thing you can do is to go see your doctor. Your doctor can try to determine what is causing your tinnitus. He or she can check to see if it is related to blood pressure, kidney function, diet, or allergies. Your doctor can also determine whether your tinnitus is related to any medicine you are taking.
To learn more about what is causing your tinnitus, your doctor may refer you to an otolaryngologist Dr Tejal Shah, Ahmedabad,India , an ear, nose, and throat doctor. He or she will examine your ears and your hearing to try to find out why you have tinnitus. Another hearing professional,anaudiologist , can measure your hearing. If you need a hearing aid, an audiologist can fit you with one that meets your needs.
Although there is no cure for tinnitus, scientists and doctors have discovered several treatments that may give you some relief. Not every treatment works for everyone, so you may need to try several to find the ones that help.
Treatments can include
- Hearing aids. Many people with tinnitus also have a hearing loss. Wearing a hearing aid makes it easier for some people to hear the sounds they need to hear by making them louder. The better you hear other people talking or the music you like, the less you notice your tinnitus.
- Maskers. Maskers are small electronic devices that use sound to make tinnitus less noticeable. Maskers do not make tinnitus go away, but they make the ringing or roaring seem softer. For some people, maskers hide their tinnitus so well that they can barely hear it.
Some people sleep better when they use maskers. Listening to static at a low volume on the radio or using bedside maskers can help. These are devices you can put by your bed instead of behind your ear. They can help you ignore your tinnitus and fall asleep. - Medicine or drug therapy. Some medicines may ease tinnitus. If your doctor prescribes medicine to treat your tinnitus, he or she can tell you whether the medicine has any side effects.
- Tinnitus retraining therapy. This treatment uses a combination of counseling and maskers. Otolaryngologists and audiologists help you learn how to deal with your tinnitus better. You may also use maskers to make your tinnitus less noticeable. After a while, some people learn how to avoid thinking about their tinnitus. It takes time for this treatment to work, but it can be very helpful.
- Counseling. People with tinnitus may become depressed. Talking with a counselor or people in tinnitus support groups may be helpful.
- Relaxing. Learning how to relax is very helpful if the noise in your ears frustrates you. Stress makes tinnitus seem worse. By relaxing, you have a chance to rest and better deal with the sound.
Think about things that will help you cope. Many people find listening to music very helpful. Focusing on music might help you forget about your tinnitus for a while. It can also help mask the sound. Other people like to listen to recorded nature sounds, like ocean waves, the wind, or even crickets.
Avoid anything that can make your tinnitus worse. This includes smoking, alcohol, and loud noise. If you are a construction worker, an airport worker, or a hunter, or if you are regularly exposed to loud noise at home or at work, wear ear plugs or special earmuffs to protect your hearing and keep your tinnitus from getting worse.
If it is hard for you to hear over your tinnitus, ask your friends and family to face you when they talk so you can see their faces. Seeing their expressions may help you understand them better. Ask people to speak louder, but not shout. Also, tell them they do not have to talk slowly, just more clearly.
OTITIS MEDIA
Otitis media is an infection or inflammation of the middle ear. This inflammation often begins when infections that cause sore throats, colds, or other respiratory or breathing problems spread to the middle ear. These can be viral or bacterial infections. Seventy-five percent of children experience at least one episode of otitis media by their third birthday. Almost half of these children will have three or more ear infections during their first 3 years. It is estimated that medical costs and lost wages because of otitis media amount to $5 billion* a year in the United States . Although otitis media is primarily a disease of infants and young children, it can also affect adults.
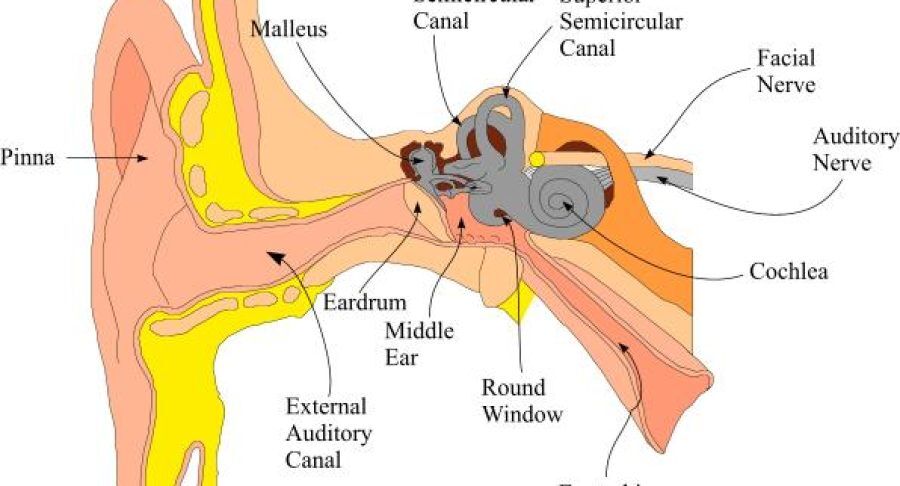
The ear consists of three major parts: the outer ear, the middle ear, and the inner ear. The outer ear includes the pinna-the visible part of the ear–and the ear canal. The outer ear extends to the tympanic membrane or eardrum,
which separates the outer ear from the middle ear. The middle ear is an air-filled space that is located behind the eardrum. The middle ear contains three tiny bones, the malleus, incus, and stapes, which transmit sound from the eardrum to the inner ear. The inner ear contains the hearing and balance organs. The cochlea contains the hearing organ which converts sound into electrical signals which are associated with the origin of impulses carried by nerves to the brain where their meanings are appreciated.
There are many reasons why children are more likely to suffer from otitis media than adults. First, children have more trouble fighting infections. This is because their immune systems are still developing. Another reason has to do with the child’s eustachian tube. The eustachian tube is a small passageway that connects the upper part of the throat to the middle ear. It is shorter and straighter in the child than in the adult. It can contribute to otitis media in several ways.
The eustachian tube is usually closed but opens regularly to ventilate or replenish the air in the middle ear. This tube also equalizes middle ear air pressure in response to air pressure changes in the environment. However, a eustachian tube that is blocked by swelling of its lining or plugged with mucus from a cold or for some other reason cannot open to ventilate the middle ear. The lack of ventilation may allow fluid from the tissue that lines the middle ear to accumulate. If the eustachian tube remains plugged, the fluid cannot drain and begins to collect in the normally air-filled middle ear.
One more factor that makes children more susceptible to otitis media is that adenoids in children are larger than they are in adults. Adenoids are composed largely of cells (lymphocytes) that help fight infections. They are positioned in the back of the upper part of the throat near the eustachian tubes. Enlarged adenoids can, because of their size, interfere with the eustachian tube opening. In addition, adenoids may themselves become infected, and the infection may spread into the eustachian tubes.
Bacteria reach the middle ear through the lining or the passageway of the eustachian tube and can then produce infection, which causes swelling of the lining of the middle ear, blocking of the eustachian tube, and migration of white cells from the bloodstream to help fight the infection. In this process the white cells accumulate, often killing bacteria and dying themselves, leading to the formation of pus, a thick yellowish-white fluid in the middle ear. As the fluid increases, the child may have trouble hearing because the eardrum and middle ear bones are unable to move as freely as they should. As the infection worsens, many children also experience severe ear pain. Too much fluid in the ear can put pressure on the eardrum and eventually tear it.
Otitis media not only causes severe pain but may result in serious complications if it is not treated. An untreated infection can travel from the middle ear to the nearby parts of the head, including the brain. Although the hearing loss caused by otitis media is usually temporary, untreated otitis media may lead to permanent hearing impairment. Persistent fluid in the middle ear and chronic otitis media can reduce a child’s hearing at a time that is critical for speech and language development. Children who have early hearing impairment from frequent ear infections are likely to have speech and language disabilities.
Otitis media is often difficult to detect because most children affected by this disorder do not yet have sufficient speech and language skills to tell someone what is bothering them. Common signs to look for are
- unusual irritability
- difficulty sleeping
- tugging or pulling at one or both ears
- fever
- fluid draining from the ear
- loss of balance
- unresponsiveness to quiet sounds or other signs of hearing difficulty such as sitting too close to the television or being inattentive
Specific prevention strategies applicable to all infants and children such as immunization against viral respiratory infections or specifically against the bacteria that cause otitis media are not currently available. Nevertheless, it is known that children who are cared for in group settings, as well as children who live with adults who smoke cigarettes, have more ear infections. Therefore, a child who is prone to otitis media should avoid contact with sick playmates and environmental tobacco smoke. Infants who nurse from a bottle while lying down also appear to develop otitis media more frequently. Children who have been breast-fed often have fewer episodes of otitis media. Research has shown that cold and allergy medications such as antihistamines and decongestants are not helpful in preventing ear infections. The best hope for avoiding ear infections is the development of vaccines against the bacteria that most often cause otitis media. Scientists are currently developing vaccines that show promise in preventing otitis media. Additional clinical research must be completed to ensure their effectiveness and safety.
The simplest way to detect an active infection in the middle ear is to look in the child’s ear with an otoscope, a lightinstrument that allows the physician to examine the outer earand the eardrum. Inflammation of the eardrum indicates aninfection. There are several ways that a physician checks for middle ear fluid. The use of a special type of otoscopecalled a pneumatic otoscope allows the physician to blow a puff of air onto the eardrum to test eardrum movement. (An eardrum with fluid behind it does not move as well as an eardrum with air behind it.)
A useful test of middle ear function is called tympanometry. This test requires insertion of a small soft plug into the opening of the child’s ear canal. The plug contains a speaker, a microphone, and a device that is able to change the air pressure in the ear canal, allowing for several measures of the middle ear. The child feels air pressure changes in the ear or hears a few brief tones. While this test provides information on the condition of the middle ear, it does not determine how well the child hears. A physician may suggest a hearing test for a child who has frequent ear infections to determine the extent of hearing loss. The hearing test is usually performed by an audiologist, a person who is specially trained to measure hearing.
Many physicians recommend the use of an antibiotic (a drug that kills bacteria) when there is an active middle ear infection. If a child is experiencing pain, the physician may also recommend a pain reliever. Following the physician’s instructions is very important. Once started, the antibiotic should be taken until it is finished. Most physicians will have the child return for a followup examination to see if the infection has cleared.
Unfortunately, there are many bacteria that can cause otitis media, and some have become resistant to some antibiotics. This happens when antibiotics are given for coughs, colds, flu, or viral infections where antibiotic treatment is not useful. When bacteria become resistant to antibiotics, those treatments are then less effective against infections. This means that several different antibiotics may have to be tried before an ear infection clears. Antibiotics may also produce unwanted side effects such as nausea, diarrhea, and rashes.**
Once the infection clears, fluid may remain in the middle ear for several months. Middle ear fluid that is not infected often disappears after 3 to 6 weeks. Neither antihistamines nor decongestants are recommended as helpful in the treatment of otitis media at any stage in the disease process. Sometimes physicians will treat the child with an antibiotic to hasten the elimination of the fluid. If the fluid persists for more than 3 months and is associated with a loss of hearing, many physicians suggest the insertion of “tubes” in the affected ears. This operation, called a myringotomy, can usually be done on an outpatient basis by a surgeon, who is usually an otolaryngologist (a physician who specializes in the ears, nose, and throat). While the child is asleep under general anesthesia, the surgeon makes a small opening in the child’s eardrum. A small metal or plastic tube is placed into the opening in the eardrum. The tube ventilates the middle ear and helps keep the air pressure in the middle ear equal to the air pressure in the environment. The tube normally stays in the eardrum for 6 to 12 months, after which time it usually comes out spontaneously. If a child has enlarged or infected adenoids, the surgeon may recommend removal of the adenoids at the same time the ear tubes are inserted. Removal of the adenoids has been shown to reduce episodes of otitis media in some children, but not those who are under 4 years of age. Research, however, has shown that removal of a child’s tonsils does not reduce occurrences of otitis media. Tonsillotomy and adenoidectomy may be appropriate for reasons other than middle ear fluid.
Hearing should be fully restored once the fluid is removed. Some children may need to have the operation again if the otitis media returns after the tubes come out. While the tubes are in place, water should be kept out of the ears. Many physicians recommend that a child with tubes wear special ear plugs while swimming or bathing so that water does not enter the middle ear.
DEAFNESS
The following questions will help you determine if you need to have your hearing evaluated by a medical professional:
Do you have a problem hearing over the telephone?
Yes No
Do you have trouble following the conversation when two or more people are talking at the same time?
Yes No
Do people complain that you turn the TV volume up too high?
Yes No
Do you have to strain to understand conversation?
Yes No
Do you have trouble hearing in a noisy background?
Yes No
Do you find yourself asking people to repeat themselves?
Yes No
Do many people you talk to seem to mumble (or not speak clearly)?
Yes No
Do you misunderstand what others are saying and respond inappropriately?
Yes No
Do you have trouble understanding the speech of women and children?
Yes No
Do people get annoyed because you misunderstand what they say?
Yes No
If you answered “yes” to three or more of these questions, you may want to see an otolaryngologist (an ear, nose, and throat specialist) or an audiologist for a hearing evaluation.
HEARING AIDS
There are three basic styles of hearing aids. The styles differ by size, their placement on or inside the ear, and the degree to which they amplify sound (see figure on page 1).
- Behind-the-ear (BTE) hearing aids consist of a hard plastic case worn behind the ear and connected to a plastic earmold that fits inside the outer ear. The electronic parts are held in the case behind the ear. Sound travels from the hearing aid through the earmold and into the ear. BTE aids are used by people of all ages for mild to profound hearing loss.
- A new kind of BTE aid is an open-fit hearing aid. Small, open-fit aids fit behind the ear completely, with only a narrow tube inserted into the ear canal, enabling the canal to remain open. For this reason, open-fit hearing aids may be a good choice for people who experience a buildup of earwax, since this type of aid is less likely to be damaged by such substances. In addition, some people may prefer the open-fit hearing aid because their perception of their voice does not sound “plugged up.”
- In-the-ear (ITE) hearing aids fit completely inside the outer ear and are used for mild to severe hearing loss. The case holding the electronic components is made of hard plastic. Some ITE aids may have certain added features installed, such as a telecoil. A telecoil is a small magnetic coil that allows users to receive sound through the circuitry of the hearing aid, rather than through its microphone. This makes it easier to hear conversations over the telephone. A telecoil also helps people hear in public facilities that have installed special sound systems, called induction loop systems. Induction loop systems can be found in many churches, schools, airports, and auditoriums. ITE aids usually are not worn by young children because the casings need to be replaced often as the ear grows.
- Canal aids fit into the ear canal and are available in two styles. The in-the-canal (ITC) hearing aid is made to fit the size and shape of a person’s ear canal. A completely-in-canal (CIC) hearing aid is nearly hidden in the ear canal. Both types are used for mild to moderately severe hearing loss.
- Because they are small, canal aids may be difficult for a person to adjust and remove. In addition, canal aids have less space available for batteries and additional devices, such as a telecoil. They usually are not recommended for young children or for people with severe to profound hearing loss because their reduced size limits their power and volume.
A hearing aid is a small electronic device that you wear in or behind your ear. It makes some sounds louder so that a person with hearing loss can listen, communicate, and participate more fully in daily activities. A hearing aid can help people hear more in both quiet and noisy situations. However, only about one out of five people who would benefit from a hearing aid actually uses one.
A hearing aid has three basic parts: a microphone, amplifier, and speaker. The hearing aid receives sound through a microphone, which converts the sound waves to electrical signals and sends them to an amplifier. The amplifier increases the power of the signals and then sends them to the ear through a speaker.
Hearing aids are primarily useful in improving the hearing and speech comprehension of people who have hearing loss that results from damage to the small sensory cells in the inner ear, called hair cells. This type of hearing loss is called sensorineural hearing loss. The damage can occur as a result of disease, aging, or injury from noise or certain medicines.
A hearing aid magnifies sound vibrations entering the ear. Surviving hair cells detect the larger vibrations and convert them into neural signals that are passed along to the brain. The greater the damage to a person’s hair cells, the more severe the hearing loss, and the greater the hearing aid amplification needed to make up the difference. However, there are practical limits to the amount of amplification a hearing aid can provide. In addition, if the inner ear is too damaged, even large vibrations will not be converted into neural signals. In this situation, a hearing aid would be ineffective.
Hearing aids work differently depending on the electronics used. The two main types of electronics are analog and digital.
Analog aids convert sound waves into electrical signals, which are amplified. Analog/adjustable hearing aids are custom built to meet the needs of each user. The aid is programmed by the manufacturer according to the specifications recommended by your audiologist. Analog/programmable hearing aids have more than one program or setting. An audiologist can program the aid using a computer, and the user can change the program for different listening environments—from a small, quiet room to a crowded restaurant to large, open areas, such as a theater or stadium. Analog/programmable circuitry can be used in all types of hearing aids. Analog aids usually are less expensive than digital aids.
Digital aids convert sound waves into numerical codes, similar to the binary code of a computer, before amplifying them. Because the code also includes information about a sound’s pitch or loudness, the aid can be specially programmed to amplify some frequencies more than others. Digital circuitry gives an audiologist more flexibility in adjusting the aid to a user’s needs and to certain listening environments. These aids also can be programmed to focus on sounds coming from a specific direction. Digital circuitry can be used in all types of hearing aids.
If you think you might have hearing loss and could benefit from a hearing aid, visit your physician, who may refer you to an otolaryngologist or audiologist. An otolaryngologist is a physician who specializes in ear, nose, and throat disorders and will investigate the cause of the hearing loss. An audiologist is a hearing health professional who identifies and measures hearing loss and will perform a hearing test to assess the type and degree of loss.
Hearing aids take time and patience to use successfully. Wearing your aids regularly will help you adjust to them.
Become familiar with your hearing aid’s features. With your audiologist present, practice putting in and taking out the aid, cleaning it, identifying right and left aids, and replacing the batteries. Ask how to test it in listening environments where you have problems with hearing. Learn to adjust the aid’s volume and to program it for sounds that are too loud or too soft. Work with your audiologist until you are comfortable and satisfied.
You may experience some of the following problems as you adjust to wearing your new aid.
- My hearing aid feels uncomfortable. Some individuals may find a hearing aid to be slightly uncomfortable at first. Ask your audiologist how long you should wear your hearing aid while you are adjusting to it.
- My voice sounds too loud. The “plugged-up” sensation that causes a hearing aid user’s voice to sound louder inside the head is called the occlusion effect, and it is very common for new hearing aid users. Check with your audiologist to see if a correction is possible. Most individuals get used to this effect over time.
- I get feedback from my hearing aid. A whistling sound can be caused by a hearing aid that does not fit or work well or is clogged by earwax or fluid. See your audiologist for adjustments.
- I hear background noise. A hearing aid does not completely separate the sounds you want to hear from the ones you do not want to hear. Sometimes, however, the hearing aid may need to be adjusted. Talk with your audiologist.
- I hear a buzzing sound when I use my cell phone. Some people who wear hearing aids or have implanted hearing devices experience problems with the radio frequency interference caused by digital cell phones. Both hearing aids and cell phones are improving, however, so these problems are occurring less often. When you are being fitted for a new hearing aid, take your cell phone with you to see if it will work well with the aid.
Before you buy a hearing aid, ask your audiologist these important questions:
- What features would be most useful to me?
- What is the total cost of the hearing aid? Do the benefits of newer technologies outweigh the higher costs?
- Is there a trial period to test the hearing aids? (Most manufacturers allow a 30- to 60-day trial period during which aids can be returned for a refund.) What fees are nonrefundable if the aids are returned after the trial period?
- How long is the warranty? Can it be extended? Does the warranty cover future maintenance and repairs?
- Can the audiologist make adjustments and provide servicing and minor repairs? Will loaner aids be provided when repairs are needed?
- What instruction does the audiologist provide?
The hearing aid that will work best for you depends on the kind and severity of your hearing loss. If you have a hearing loss in both of your ears, two hearing aids are generally recommended because two aids provide a more natural signal to the brain. Hearing in both ears also will help you understand speech and locate where the sound is coming from.
You and your audiologist should select a hearing aid that best suits your needs and lifestyle. Price is also a key consideration because hearing aids range from hundreds to several thousand dollars. Similar to other equipment purchases, style and features affect cost. However, don’t use price alone to determine the best hearing aid for you. Just because one hearing aid is more expensive than another does not necessarily mean that it will better suit your needs.
A hearing aid will not restore your normal hearing. With practice, however, a hearing aid will increase your awareness of sounds and their sources. You will want to wear your hearing aid regularly, so select one that is convenient and easy for you to use. Other features to consider include parts or services covered by the warranty, estimated schedule and costs for maintenance and repair, options and upgrade opportunities, and the hearing aid company’s reputation for quality and customer service
Proper maintenance and care will extend the life of your hearing aid. Make it a habit to:
- Keep hearing aids away from heat and moisture.
- Clean hearing aids as instructed. Earwax and ear drainage can damage a hearing aid.
- Avoid using hairspray or other hair care products while wearing hearing aids.
- Turn off hearing aids when they are not in use.
- Replace dead batteries immediately.
- Keep replacement batteries and small aids away from children and pets.
Although they work differently than the hearing aids described above, implantable hearing aids are designed to help increase the transmission of sound vibrations entering the inner ear. A middle ear implant (MEI) is a small device attached to one of the bones of the middle ear. Rather than amplifying the sound traveling to the eardrum, an MEI moves these bones directly. Both techniques have the net result of strengthening sound vibrations entering the inner ear so that they can be detected by individuals with sensorineural hearing loss.
A bone-anchored hearing aid (BAHA) is a small device that attaches to the bone behind the ear. The device transmits sound vibrations directly to the inner ear through the skull, bypassing the middle ear. BAHAs are generally used by individuals with middle ear problems or deafness in one ear. Because surgery is required to implant either of these devices, many hearing specialists feel that the benefits may not outweigh the risks.
